Hi! This is Rita Shushy Setrakian, Kate Scarlata’s intern for the next few weeks. I am a dietetic intern at Teachers College, Columbia University, where I also earned my Master’s of Science in nutrition education. I’m here to share a low FODMAP recipe with you using firm tofu! But before we get to cooking, let’s […]
Continue ReadingFODMAPs
 Bloating: Potential Causes and Treatments + a Book Giveaway!
Bloating: Potential Causes and Treatments + a Book Giveaway!
I thought I would talk about bloating today. Does that sound like a good plan? Abdominal bloating is a common clinical problem, and I would say, it is one of the most bothersome symptom in individuals with IBS. What contributes to bloating? “Four factors are involved in the pathophysiology of bloating: a subjective sensation of […]
Continue Reading
 Low FODMAP Cooking + Learning with Chef Ming Tsai and Dietitian Kate Scarlata
Low FODMAP Cooking + Learning with Chef Ming Tsai and Dietitian Kate Scarlata
Upcoming Low FODMAP tasting with celebrity chef, Ming Tsai and dietitian, Kate Scarlata on November 7, 2018 from 7-9 PM in Boston!
Continue Reading
 One Skillet BBQ Chicken
One Skillet BBQ Chicken
You’ll love this super easy low FODMAP BBQ chicken recipe made with Casa de Sante’s BBQ Rub!
Continue Reading
 Berry Cobbler (gluten free + low FODMAP)
Berry Cobbler (gluten free + low FODMAP)
Delicious berry cobbler made with love for those with a sensitive belly.
Continue Reading
 New Low FODMAP Product: Happy Hot Jerky
New Low FODMAP Product: Happy Hot Jerky
Rachel Pauls Food launches all new low FODMAP protein rich snack option–Happy Hot Jerky!
Continue Reading
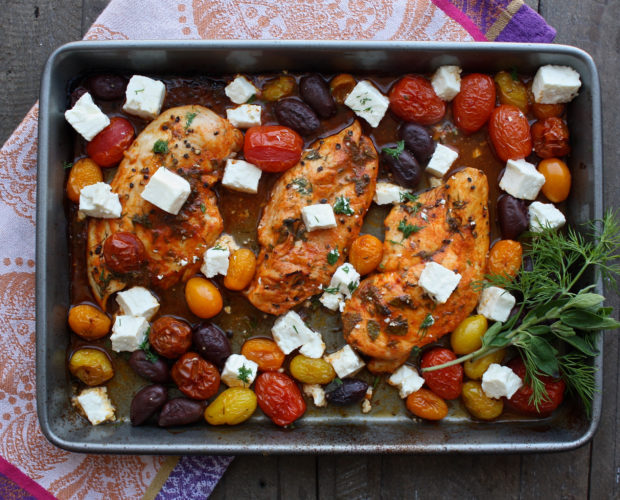 One Pan Greek Chicken with Feta, Olives + Tomatoes
One Pan Greek Chicken with Feta, Olives + Tomatoes
One pan Greek Chicken! Get ready for a mouthful of delicious flavor without the FODMAPs.
Continue Reading
 One Pan Roasted Shrimp Adobo with Tomatoes and Green Beans
One Pan Roasted Shrimp Adobo with Tomatoes and Green Beans
Flavorful one pan meal: roasted shrimp seasoned with Casa de Sante’s Adobo Seasoning and a side of colorful low FODMAP veggies!
Continue Reading
 I Believe in Your Story Campaign
I Believe in Your Story Campaign
April is IBS Awareness Month. I hope you join the mission of the #IBelieveinyourStory campaign.
Continue Reading
